FAU students report long wait times at CAPS
Staff at FAU’s Counseling and Psychological Services are outnumbered 1-to-1,364 as students report lengthy wait times for their mental health services.
January 18, 2023
Students say they have encountered longer wait times for counseling services during the Fall 2022 semester, after Florida Atlantic University welcomed the largest freshman class in its history.
With 22 clinical staff members and 30,000 students across its three campuses, the staff-to-student ratio at FAU’s counseling center is 1-to-1,364. This ratio falls within the standard set by International Accreditation of Counseling Services (IACS), an organization that focuses on accrediting professional counseling centers on higher academic campuses, of one counselor to every 1,000-15,000 students.
FAU also employs two psychology residents who carry the same workload as the 22 full time senior staff clinicians, three part-time doctoral interns, and four part-time licensed clinicians.
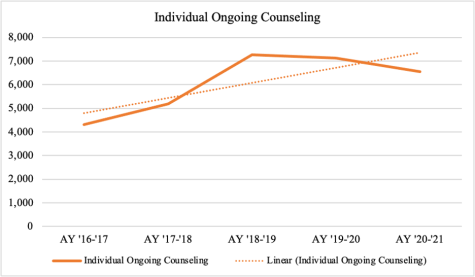
According to FAU’s Annual Reports, Counseling and Psychological Services (CAPS) satisfaction surveys report an overall increase in student participation since 2016 — following a nationwide trend of increased demand for psychological services.
Leonette Copeland, CAPS’ assistant director of outreach and consultation, explained the increase in enrollment and the growing number of students interested in utilizing their services have presented a challenge.
“If you think about how many registered students are at FAU, it would be really tough to guarantee weekly therapy and long-term therapy to all of those students,” Copeland said.
Nonetheless, the linear trendline indicates that despite variations in demand, the number of students attending long-term or “ongoing counseling” continues to increase since the 2016-17 academic year.
Institutions of higher education have provided counseling and other psychological services to students for more than 160 years. Even before the onset of pandemic stresses, universities have witnessed trends of increasing demand for long-term mental health services.
“Five to eight years pre-COVID the focus really was on year after year increase and demand on services […] that continues to be an issue,” said Scott Strader, licensed psychologist and director of the Counseling Center at the University of South Florida.
Hannah Tuttle, a senior majoring in physics, believes there should be long-term mental health care on campus. “I don’t see why you can’t get long-term therapy for free or a reduced price,” she said.
The origins & evolution of college counseling
CAPS’ original function in higher education was to provide short-term guidance to students as they transition away from home, into adulthood, and then into the workforce.
Counseling Psychologist Alison LaFollette, who has her own practice based in Salt Lake City, Utah, claims the demands of college students have changed significantly since they are increasingly looking for long-term services.
Dr. David Kraft, a psychiatrist based in Massachusetts, wrote in a 2011 paper that the counseling model changed once universities began to accept veterans and realized students were abusing drugs and alcohol.
Justine Kantor, a sophomore criminal justice major and director of Psychoeducational Programming within the university’s student government, expressed concerns of drug and alcohol abuse.
“That’s what I’ve noticed to be a big factor in mental health declining. [Students are] not leaving their rooms, and they’re sitting in there and they’re smoking weed all day,” Kantor said.
Strader and Kantor referenced COVID-19 as a primary factor for the noticed uptick in student visitation. Students’ hesitation to intimately engage with one another post-COVID has resulted in high levels of loneliness, according to Kantor.
Copeland suggested that social movements normalizing conversations surrounding mental health on and off campuses have encouraged mental health transparency and communication, resulting in what may appear to be an uptick in mental illness amongst the college population.
“I don’t know if I’m seeing an increase, as if it’s things that are more of a problem, or if we’ve done really well [destigmatizing mental health] that you just have more people willing to talk about it,” Copeland said.
The convenience and accessibility of mental health care on campus attracts students who may not have the resources like health insurance to outsource care.
Psychiatrists Dr. Victor Schwartz, from New York University, and Dr. Jerald Kay, from Wright State University, wrote in a 2009 paper that the use of campus counseling and psychological services as a primary source of health care has also been a factor to the issue where student demand has “outpaced the capacity and rate of growth” of school counseling.
Student perspective on the crisis
Tuttle first chose to use CAPS for its free service when other therapy options were expensive.
She said service at CAPS was great and wait times were not bad at first. That changed during the summer of her freshman year when CAPS decreased the frequency of her sessions from an hour-long weekly visit to a half-hour biweekly visit while her symptoms were worsening.
Staff members ultimately referred Tuttle out of the Counseling Center.
“They told me they couldn’t deal with the severity of my issues,” she said.
Tuttle shared that the counseling center staff explained they are based on short-term specific therapy and not designed to deal with mood disorders like depression.
“The reason we work from a shorter-term model is because our services are supposed to be accessible to registered students,” Copeland said.
Tuttle believes being referred out was better in the long term because she has “a stronger network of people,” but she was worried about affording therapy at the time.
Kyrie Bradley, a senior political science major, has been using CAPS for two semesters and noticed an uptick in wait times this semester.
“I’ve gone sometimes three weeks without meeting with a CAPS’ adviser and that’s been a bit of a hassle to try and get around when CAPS is incredibly helpful as a service, and when it’s restricted like that, it becomes a hindrance,” Bradley said.
When first-time students request an appointment at CAPS, they get it within the week of their initial request, according to Copeland. Students, however, have criticized the wait time to get a follow-up appointment.
Tuttle said her boyfriend got an initial appointment the week he requested one from CAPS, but then had to wait seven months for a second appointment with a professional.
“I think there may be either not enough therapists or too much demand, because every time we checked online there were no appointments. And we checked in person several times and there were no appointments,” she said.
Copeland mentions that the field of counseling in general is susceptible to staff turnover.
“Even if you have a full staff fall, by the end of spring people might be like ‘I want to move to California,’ so you may not always maintain [staff],” Copeland said.
Heather Saunders is a postdoctoral fellow at the Program on Medicaid and the Uninsured at the Kaiser Family Foundation, a non-partisan, nonprofit organization focusing on analysis of health policy, public health, and national health issues.
Saunders said the prevalence of mental illness in the university setting is high, but often time goes untreated.
People between the ages of 18 and 25 have the highest prevalence of mental illness and substance use disorders out of all age groups, according to Saunders.
“Even though the prevalence of mental illness is the highest of any group, they are the least likely to receive treatment,” Saunders said. “Only 45% of people with mental illness between the ages of 18 to 25 receive treatment compared to 61% of adults overall.”
Saunders partly attributed the deficit of treatment in this age group to the lack of insurance. She said the rate of uninsured individuals is highest amongst young adults between the ages of 19 and 34. She also mentioned the difficulty navigating the healthcare system and the workforce shortage as possible contributors.
“Even when people do reach out for help, it’s difficult for them to find and access treatment,” she said.
According to Saunders, the lack of accessible treatment for mentally ill students often results in worsening symptoms, secondary diagnosis, low GPA and high dropout rates. Her research shows that one in four university students report suicidal ideation and 9% report attempted suicide, and trends indicate these statistics are on the rise.
Editor’s note: This story is in the UP’s latest issue that can be found physically on the distribution boxes around campus or digitally through our Issuu page.
Jasmine Die is the Copy Desk Chief for the University Press. For more information regarding this or other stories, email [email protected].
















